All you need to know about what is in a cigarette, how it is made, and what is in the cigarette smoke
- the composition of a cigarette
- what is in cigarette smoke
- the amount of nicotine in a cigarette

All you need to know about what is in a cigarette, how it is made, and what is in the cigarette smoke

In this section, you will find several articles explaining everything you need to know about nicotine: a test to help you determine how much nicotine you need, the amount of nicotine in a cigarette, the optimal nicotine concentration for your e-liquids, and the effects of nicotine on health, nicotine salts.

E-cigarettes are often presented as a safer alternative to traditional cigarettes. But how do they truly compare across the spectrum of our health? Let’s delve into the known effects, always drawing comparisons to the harms of combustible tobacco.
One of the initial appeals of e-cigarettes lies in their diverse flavor profiles, ranging from tobacco to mint to fruits to desserts, a stark contrast to the often harsh, smoky taste of traditional cigarettes. E-cigarettes offer a “throat hit” that mimics smoking, it’s produced by nicotine. Traditional cigarettes deliver this sensation through the burning of tobacco and the inhalation of hot smoke and tar.
Switching to e-cigarettes generally leads to an improvement in breath odor compared to the persistent stale smell associated with cigarette smoking. The tar and chemicals in traditional cigarettes famously stain teeth and contribute to gum disease and halitosis (bad breath). E-cigarettes still contain nicotine, xxx.
Traditional cigarettes are notorious for their devastating impact on the lungs, causing chronic bronchitis, emphysema, and a dramatically increased risk of lung cancer. They introduce thousands of chemicals, including known carcinogens, directly into the delicate lung tissue. E-cigarettes, while free of tobacco combustion byproducts like tar and carbon monoxide, are not harmless to the lungs. The heated aerosols contain xxx. These can cause xxx.
Traditional cigarettes pose significant risks to the heart and circulatory system. This chronic stress on the cardiovascular system can lead to an increased risk of heart attacks and strokes. Traditional cigarettes compound this risk with carbon monoxide, which reduces the blood’s oxygen-carrying capacity, and other chemicals that promote atherosclerosis (hardening of the arteries). While e-cigarettes eliminate carbon monoxide, xxx.
Addiction
Mood
Nicotine’s impact on neurotransmitters can affect mood regulation, potentially contributing to or worsening feelings of depression and anxiety, rather than alleviating them.
Traditional cigarettes are a leading cause of cancer, responsible for cancers of the lung, throat, mouth, esophagus, bladder, and many others, due to the myriad of carcinogens produced during combustion. E-cigarettes, by contrast, do not involve combustion and therefore eliminate exposure to many of the tar and tobacco-specific carcinogens found in traditional smoke. However, xxx. The full extent of this risk is still under investigation.
Smoking traditional cigarettes is known to suppress appetite and increase metabolism, leading to a tendency for smokers to weigh less than non-smokers. Consequently, quitting smoking often results in weight gain, a significant concern for many who are trying to quit. Nicotine in e-cigarettes also has appetite-suppressing effects. Therefore, the overall health benefits of avoiding traditional cigarettes far outweigh potential concerns about weight changes.
Traditional cigarette smoking poses serious risks during conception, pregnancy, and breastfeeding. For fertility, smoking can negatively impact both male and female reproductive health, making conception more difficult. During pregnancy, exposure to smoke can lead to complications such as premature birth, low birth weight, and developmental issues in the fetus. During breastfeeding, nicotine passes into breast milk, which can affect the infant’s sleep patterns, heart rate, and overall well-being. While traditional cigarettes introduce thousands of additional harmful chemicals beyond nicotine, the presence of nicotine in e-cigarettes still makes them a significant concern for pregnant and breastfeeding mothers.
Interestingly, nicotine itself, separate from the harmful delivery mechanisms, has shown some intriguing therapeutic potential in specific contexts. Research has explored its effects on cognitive function, attention, and memory, leading to studies on its potential role in treating conditions like Parkinson’s disease, Tourette’s syndrome, and even some aspects of Alzheimer’s disease. The mechanism involves nicotine’s interaction with specific receptors in the brain. However, it is crucial to emphasize that these are areas of ongoing scientific investigation, typically involving controlled doses of pharmaceutical-grade nicotine, not through smoking or vaping. The potential benefits are being studied in a medical context, completely detached from recreational use.
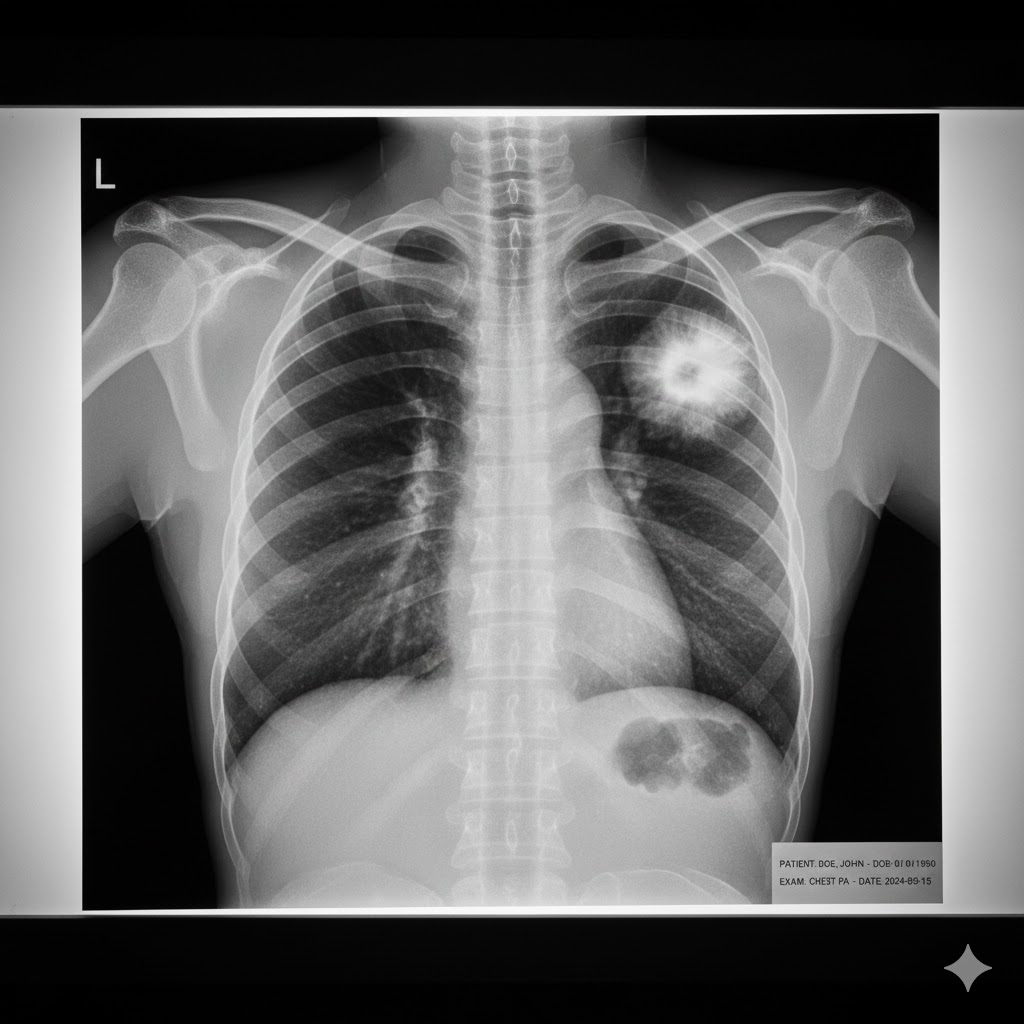
Lung cancer is the leading cause of cancer death in men and women worldwide. The most significant and controllable factor behind this devastating disease is smoking. Understanding the risks, symptoms, and consequences of lung cancer is an important and necessary step in deciding to quit smoking.
The primary cause of lung cancer is exposure to cancer-causing substances (carcinogens), which inflict damage upon the cells lining the lungs.
Smoking (Cigarettes, Cigars, Pipes) is, by far, the leading risk factor, responsible for about 80% of lung cancer deaths. The risk escalates directly with the total number of years and packs smoked. Carcinogens in tobacco smoke cause immediate and chronic changes to lung tissue; while the body attempts to repair this damage, repeated exposure ultimately causes healthy cells to begin growing out of control.
Furthermore, breathing in secondhand smoke significantly increases the risk of developing lung cancer, even for individuals who have never smoked. Radon Gas, a naturally occurring radioactive gas released from the breakdown of uranium in soil and rock, is the second-leading cause of lung cancer and the leading cause among non-smokers. It can dangerously accumulate in homes, particularly in basements. Workplace Exposures to substances like asbestos, arsenic, chromium, and nickel compounds can also heighten risk, especially for those who also smoke. Previous radiation therapy or a family history of lung cancer are also acknowledged risk factors.
While lung cancer remains a major killer, the overall number of new cases and deaths is thankfully decreasing. This positive trend is largely attributed to fewer people smoking or starting to smoke.
Lung cancer kills more people each year than breast, colon, and prostate cancers combined. The general lifetime risk of developing lung cancer is approximately 1 in 17 for men and 1 in 18 for women; however, for those who smoke, this risk is substantially higher.
The most compelling statistic is the Quitting Effect: stopping smoking, even after many years, significantly lowers your risk. The risk of developing lung cancer drops by half within 10 to 15 years after quitting. For those diagnosed with Non-Small Cell Lung Cancer (NSCLC), former smokers have a lower chance of dying compared to current smokers, and the longer the duration of cessation prior to diagnosis, the better the survival outcome.
It is important to understand that many lung cancers do not cause symptoms until they have progressed to a later stage. Seeing a doctor if you experience any of the following persistent signs is crucial for the possibility of earlier detection:
Lung cancer is mainly categorized into two groups, which require different treatment approaches:
| Type of Lung Cancer | Prevalence | Key Characteristics |
| Non-Small Cell Lung Cancer (NSCLC) | About 87% of all lung cancers. | Grows and spreads more slowly than SCLC. Includes Adenocarcinoma (most common, often found in non-smokers as well), Squamous Cell Carcinoma, and Large Cell Carcinoma. |
| Small Cell Lung Cancer (SCLC) | About 13% of all lung cancers. | Highly linked to heavy smoking; it is rare in never-smokers. It tends to grow and spread very quickly. |
If lung cancer is suspected, a combination of tests will be utilized for both diagnosis and staging (determining the extent of the cancer).
Imaging Tests such as a Chest X-ray or CT (Computed Tomography) Scan are used to identify suspicious areas. Low-Dose CT (LDCT) is the only recommended screening tool for high-risk individuals (those with a long smoking history, current smokers, or those who quit within the last 15 years, usually aged 50–80). A PET (Positron Emission Tomography) Scan is typically used to check for the spread of cancer to other parts of the body (staging).
A Biopsy is the definitive and only way to confirm a cancer diagnosis. A small sample of tissue is removed using a procedure like a bronchoscopy or a CT-guided needle biopsy. This sample is then meticulously examined under a microscope. Furthermore, Molecular Testing of the biopsy tissue is essential for advanced cases, as it checks for specific gene changes (mutations) that can inform targeted treatment options, particularly for NSCLC.
Treatment selection depends critically on the type of cancer, the stage at diagnosis, and the patient’s overall health.
| Treatment Modality | Description |
| Surgery | Often used for early-stage NSCLC to remove the tumor (e.g., lobectomy, pneumonectomy). It is rarely a primary treatment for SCLC. |
| Radiation Therapy | Uses high-energy rays to kill cancer cells. It can be used alone, before or after surgery, or in conjunction with chemotherapy. |
| Chemotherapy | Anti-cancer drugs used to destroy cancer cells throughout the body. This is a primary treatment for SCLC. |
| Targeted Therapy | Drugs that specifically attack certain gene mutations in cancer cells, often used for advanced NSCLC. |
| Immunotherapy | Drugs that stimulate the body’s own immune system to recognize and destroy cancer cells. |
| Palliative Care | Focuses on managing symptoms and improving the patient’s quality of life, especially in later stages of the disease. |
The prognosis for lung cancer is heavily influenced by the stage at which it is found. Early detection drastically improves survival odds. The statistics below are the 5-year relative survival rates (the percentage of people who live for at least 5 years after diagnosis compared to the general population).
| Overall Survival Rates (All Stages, US data) | 1-Year Survival | 5-Year Survival |
| All Lung Cancer Combined | Approx. 45% (UK data) | Approx. 29.7% (US data) |
| Survival by Stage at Diagnosis (US SEER Data) | 5-Year Survival Rate (NSCLC) | 5-Year Survival Rate (SCLC) |
| Localized (confined to the lung) | 67% | 34% |
| Regional (spread to nearby lymph nodes) | 40% | 20% |
| Distant (spread to distant organs) | 12% | 4% |
The takeaway is clear: catching the cancer when it is Localized—which often occurs through screening for high-risk individuals—results in a significantly better outcome. Quitting smoking today is the single most important action you can take to lower your risk, improve your body’s ability to heal, and increase your chances of a better prognosis if a diagnosis does occur.
Rate this article by clicking on the desired number of stars:
Please use the “Comments” field below to share your experience or suggest improvements to this article.

The CDS test
Answer these 5 questions to assess your level of addiction to cigarettes:
| Please rate your addiction to cigarettes on a scale of 0–100 | 0 = I am NOT addicted to cigarettes at all 100 = I am extremely addicted to cigarettes Addiction: 0–20 = 1 point 21–40 = 2 points 41–60 = 3 points 61–80 = 4 points 81–100 = 5 points |
| On average, how many cigarettes do you smoke per day? | Cigarette/day : 0–5 = 1 point 6–10 = 2 points 11–20 = 3 points 21–29 = 4 points 30+ = 5 points |
| Usually, how soon after waking up do you smoke your first cigarette? | Minutes : 0-5 = 5 points 6–15 = 4 points 16–30 = 3 points 31–60 = 2 points 61+ = 1 point |
| For you, quitting smoking for good would be: | Impossible = 5 points Very difficult = 4 points Fairly difficult = 3 points Fairly easy = 2 points Very easy = 1 point |
| After a few hours without smoking, I feel an irresistible urge to smoke | Totally disagree = 1 point Somewhat disagree =2 points Neither agree nor disagree = 3 points Somewhat agree = 4 points Fully agree = 5 points |
Now add your points (maximum=25)
Interpretation :
5-10 points: Low level of addiction
11-15 points: Moderate level of addiction
16-20 points: Strong level of addiction
21-25 points: Very strong level of addiction
Our previous research found that a value of 16 or above indicates that your are strongly addicted to cigarettes.(a)
This questionnaire is called the Cigarette Dependence Scale (CDS-5), it is a well-validated measure of dependence.(b)
References:
a) Etter JF, Comparing the validity of the Cigarette Dependence Scale and the Fagerström Test for Nicotine Dependence, Drug and Alcohol Dependence, Volume 95, Issues 1–2, 2008, Pages 152-159, ISSN 0376-8716, https://doi.org/10.1016/j.drugalcdep.2008.01.017.
b) Etter, JF., Le Houezec, J. & Perneger, T. A Self-Administered Questionnaire to Measure Dependence on Cigarettes: The Cigarette Dependence Scale. Neuropsychopharmacology 28, 359–370 (2003). https://doi.org/10.1038/sj.npp.1300030
Please rate this article by clicking on the desired number of stars:
Please use the “Comments” field below to share your experience or suggest improvements to this article.