For many smokers, the link is visceral. The smell of beer or the taste of wine triggers an almost instinctive reflex to reach for a cigarette. This powerful link between tobacco and alcohol is not only a difficult habit to break, it is a synergistic threat that greatly amplifies the health risks, far beyond the sum of its parts. Understanding why these two substances are so often consumed together and the amplified dangers they create is crucial for anyone trying to break free from the grip of tobacco.
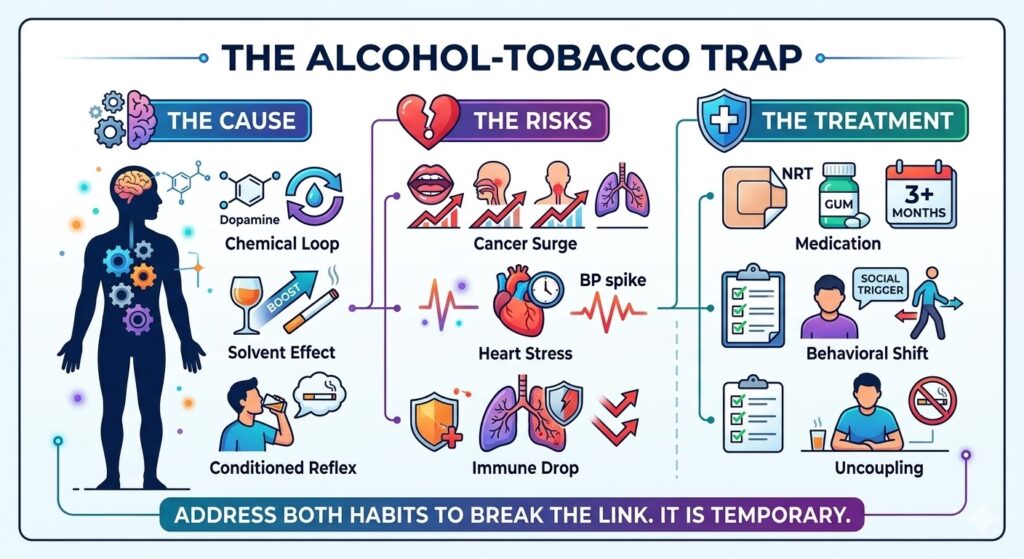
The Science of the Sinister Pair
Why do alcohol and tobacco seem so inseparable? The reason lies in the intricate interplay of chemistry and habit. Nicotine, a powerful stimulant, works on the brain’s reward pathways by releasing dopamine. Alcohol, conversely, is a central nervous system depressant. Paradoxically, alcohol can heighten the pleasant effects of nicotine while simultaneously dulling its stimulant edge. This can lead smokers to consume more cigarettes to maintain the desired effect, creating a escalating cycle. Beyond the physical, there is the powerful associative learning. Years of pairing cigarettes with drinks in social settings or during stress create potent neural pathways. The very atmosphere of a bar, or the taste of a specific beverage, becomes a signal to the brain, igniting a forceful craving.
A Compound Crisis: The Amplified Health Threats
While either habit alone is a significant health burden, consuming tobacco and alcohol together creates a compounding crisis. This synergy dramatically accelerates the risk of various cancers. Alcohol acts as a solvent, increasing the body’s absorption of the carcinogenic chemicals in tobacco smoke. Nowhere is this devastating teamwork more apparent than in cancers of the mouth, throat, and esophagus. Studies consistently show that the risk of developing these diseases is exponentially higher for combined users compared to those who only smoke or only drink. The relationship is not simply additive; it is multiplicative. Cardiovascular risks also surge. Both substances stress the heart and blood vessels—alcohol can raise blood pressure, while nicotine constricts arteries and boosts heart rate. Together, they form a perfect storm for heart attacks, strokes, and peripheral arterial disease. Respiratory diseases, too, are exacerbated, as alcohol weakens the immune response in the lungs, leaving them more vulnerable to the damage caused by tobacco smoke.
Devising a Treatment Strategy: Breaking the Double Habit
Successful cessation in the context of combined alcohol and tobacco use requires a comprehensive, integrated approach. The most effective strategies utilize a dual-pronged assault, combining pharmacological support with robust behavioral therapies. On the medication front, several options can help. Nicotine Replacement Therapies (NRT) like patches, gum, and lozenges can manage nicotine withdrawal, reducing the urge to smoke when alcohol triggers arise. Prescription medications such as Varenicline (Chantix) or Bupropion (Zyban) work differently, targeting nicotine receptors or neurotransmitters in the brain to decrease both the pleasure of smoking and the intensity of cravings. It’s essential to consult a healthcare provider to determine the safest and most suitable medication, especially if there are underlying health conditions linked to alcohol use.
The Behavioral Blueprint: Rewriting the Script
Medication provides a critical foundation, but behavioral therapy offers the essential toolkit for long-term success. Cognitive Behavioral Therapy (CBT) is highly effective, helping individuals identify the unique, interconnected triggers that link their drinking to their smoking. Individuals learn to anticipate high-risk situations—the post-work pint or the weekend gathering—and develop specific, actionable coping mechanisms. These strategies might involve developing assertive refusal skills, planning smoke-free social activities, or finding alternative ways to manage stress that don’t involve either substance. Furthermore, counseling addresses the underlying emotional drivers. Support groups provide a powerful sense of community and shared struggle. Many cessation programs now explicitly address the tobacco-alcohol link, helping participants systematically uncouple the habits. Learning to socialize without a drink in one hand and a cigarette in the other involves essentially relearning how to navigate social spaces. By developing these new skills and rewriting the ingrained behavioral script, individuals can systematically break the chain that binds tobacco and alcohol.
Use the ‘Comments’ field below to share your experience or to suggest improvements to this page.


Leave a Reply